The Bugs Are Going To Win… Or not?
/First of all, our apologies for being AWOL for the last several weeks. We were on deadline on the developmental edit of LONE WOLF and barely had time to sleep, let alone come up with a well-researched article for the blog. But the manuscript is done now, and handed in, and we’re back in business!
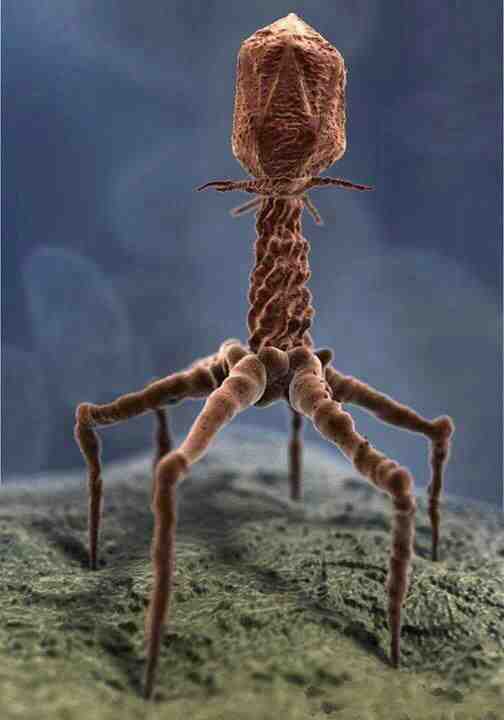
A T4 bacteriophage poised to infect a bacterium.
I have a saying that I seem to repeat often: “The bugs are going to win.” This refers to the oncoming crisis humankind is likely to have against microbes (or ‘bugs’ as we generically refer to bacteria in the lab). In a day and age when factory-farmed animals are given antibiotics prophylactically and too many medical professionals still consider knee-jerk prescription writing for antibiotics an acceptable act, news stories repeatedly warn of the number of strains of bacteria resistant to all antibiotics. Another continual theme are reports of now-resistant bacteria that used to be susceptible to a shrinking number of heavy hitting antibiotics used in only the most severe hospital cases.
In many ways, the thought of these tiny organisms taking out human kind is hard to wrap your brain around. We’re the top of the food chain; we have technology and science on our side. How can they top that? Part of the answer is very simple—replication rate. Your average bacteria divides into two identical daughter cells approximately every 20 minutes. It takes humans approximately 20 years for that same replication. This rate of bacterial replication leads to a very large number of progeny—in one day, a single bacterium can produce 4.7 x 10^21 bacteria. Even if the mutation rate is only 1 in 10^10 DNA base pairs, depending on the genome size of the bacteria, hundreds of mutations can occur in a span of less than 10 hours. Some of these mutations could lead to an inactive bacterium, but one of them might lead to a new gene conferring resistance to one of our last ditch antibiotics.
What happens when we can no longer control bacteria with a pill or injection and we enter the post-antibiotic age? It will be like going back to the early 20th century, before the advent of penicillin. Pneumonia would be a fatal infection. Bacterial epidemics similar to the Black plague that killed 30 million people—a full third of Europe at the time—could once again be a scenario faced by the world. Those who are very young and very old will be at risk due to compromised or immature immune systems. It’s a very scary concept.
So how can we beat the bugs?
- Develop new chemical therapies or multi-therapies: Scientists at Merck Research Laboratories in New Jersey recently announced two separate compounds, tarocin A and tarocin B, that makes Methicillin-resistant Staphylococcus aureaus (MRSA; a bacteria well known for its resistance) susceptible to antibiotics again. Tarocins A and B target the bacterial cell wall, and, when used with standard antibiotics, kill the bacteria effectively in mice. Human trials will be the next test.
- Find new natural anti-bacterial compounds: Dr. Gerry Wright at McMaster University has been sending students around North America to sample soil in different areas. Compounds from those soils are then tested against bacteria. If the bacteria are killed, the samples are then further tested to determine the successful compound. So far the team has made two notable discoveries:
- AMA, a molecule produced by a fungus in Nova Scotia soil that is able to knock out one of the strongest and most worrisome antibiotic resistance genes, NDM-1. NDM-1 is such a concern that the World Health Organization identifies it as a global health threat. When AMA is used, regular antibiotics once again become effective.
- Teixobactin is an antimicrobial molecule produced by one bacteria to kill others and was discovered in the soil from a field in Maine. The compound has been shown to be effective in killing multiple antibiotic resistant strains of bacteria.
- Revisit OLD remedies: A one thousand year-old Anglo Saxon recipe to treat eye infections using onion, garlic, wine and cow bile has been found by modern scientists to kill MRSA. Rather than being any individual ingredient that was effective, it was the combined recipe that killed 90% of the MRSA in the sample.
- Use their own natural enemies against them: We’re all familiar with the concept of viruses. Bacteriophage are viruses that attack bacteria (see the above photo), acting as all viruses do—they inject their contents into the bacterium and highjack it’s replication machinery to produce hundreds or thousands of copies of itself, eventually bursting the bacterium, killing it. Scientists in Russia and parts of Europe have used bacteriophage for nearly a century as antibacterials. The Western world is now looking at phage therapy as a potential replacement for antibiotics.
In the end, the question remains can we beat the bugs, and that remains to be seen. In the meantime, be conscientious citizens of the world. Do not demand antibiotics for your kids because they have ear infections, of which a full 70% can be caused by viruses; wait and let the infection run its course and it will likely clear up just as fast without antibiotic usage. Don’t run to the doctor every time you have a cold until you hit the 7 to 10 day range and a secondary infection may have set in. We should only use antibiotics when they are truly necessary. And maybe, just maybe, the bugs won’t win after all.
Photo credit: Xvivo Scientific Animation



 43.0%
43.0%